Is your seltzer habit harming your teeth?
By Caitlin Dow

Sparkling water has all the bubbly and none of the sugar of soda. But is there a downside?
“Sparkling water is made by pumping carbon dioxide into water,” explains John Ruby, a retired professor of pediatric dentistry at the University of Alabama, Birmingham. “The CO2 turns into carbonic acid, and the pH drops.”
A lower pH means that the liquid has become more acidic. (Pure water has a neutral pH of 7 on the 0-to-14 pH scale.)
Acids can erode tooth enamel. And “once you lose enamel, you never get it back,” says Ruby. That can lead to sensitivity, discoloration, and loss of tooth structure.
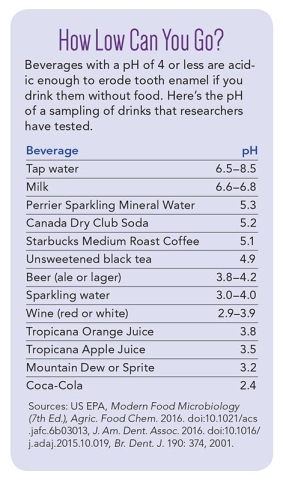
“Erosion doesn’t occur above pH 4,” Ruby explains. “A pH of 3 to 4 is erosive, and 2 to 3 is extremely erosive.” (Colas are around 2.4.)

Seltzer or sparkling water with nothing added has a pH between 3 and 4, so either may damage your enamel. But drinking them with food raises the pH of what’s in your mouth. “So it’s largely a problem if you’re drinking them alone,” says Ruby.
How much of a problem?
No long-term studies have looked at enamel erosion in the teeth of sparkling-water drinkers.
And club soda and carbonated mineral water (like plain San Pellegrino or Perrier) have added or naturally occurring minerals, which raise the pH to about 5, well outside the erosion zone.

One question mark: flavorings.
“When companies start adding citric acid to carbonated water or citric or phosphoric acid to soft drinks, we’re in a different ballpark,” says Ruby, “because that drops the pH.”
Many flavored waters have two ingredients: carbonated water and natural flavors. Citric acid could be a component of one of those “flavors,” but labels don’t have to list it separately, so consumers would never know.
“There are naturally occurring citric acids in many citrus flavors,” LaCroix told us. “However, the levels in the finished product are extremely low,” and LaCroix is “less acidic than traditional soft drinks.” (The company wouldn’t give us pH levels for its waters.)
Tips for sparkling-water fans:
- Don’t brush your teeth for at least 30 minutes after drinking. “The acid in the sparkling water softens up the surface of the tooth,” Ruby explains. “That makes your teeth more sensitive to abrasion. The last thing you want to do is brush them.”
- Don’t sip all day without food. The longer acids are in contact with your teeth, the more damage they do.
- Beware if you have dry mouth. Saliva helps neutralize acid, so think twice about the bubbly if you have dry mouth.
The Bottom Line
Sparkling water is less acidic—and less sugary—than soda. It’s not clear how much sparkling water is enough to erode your enamel, but if you’re worried, don’t overdo it.


:max_bytes(150000):strip_icc():format(webp)/GettyImages-158953264-584b0dae3df78c491e2456ec.jpg)